For Silvia Mahumane, advocacy is personal. A social activist and human rights defender, she has dedicated her career to ensuring sex workers in Mozambique are recognised, respected, and protected.
“I work to defend the rights of sex workers in the face of the stigma and discrimination they experience every day,” she says.
Mozambique remains among the countries most affected by HIV in Southern Africa. According to the U.S. Centres for Disease Control and Prevention (CDC), adult HIV prevalence in Mozambique was estimated at 11.5% in 2023. Nearly 2 million people were receiving antiretroviral therapy (ART) that year, reflecting both the magnitude of the epidemic and progress in treatment accessibility.
For sex workers, the burden is even heavier. A 2025 modelling study published in BMC Public Health found that female sex workers and their sexual partners account for roughly 5.2% of new HIV infections in the country.
Before funding cuts disrupted essential programmes, sex workers benefited from a robust network of community-led services.
“Before the funding was suspended, we conducted outreach, public awareness, and educational activities on HIV, violence against key populations, reporting mechanisms, and referrals to HIV care, treatment, and prevention services,” Mahumane explains.
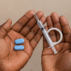
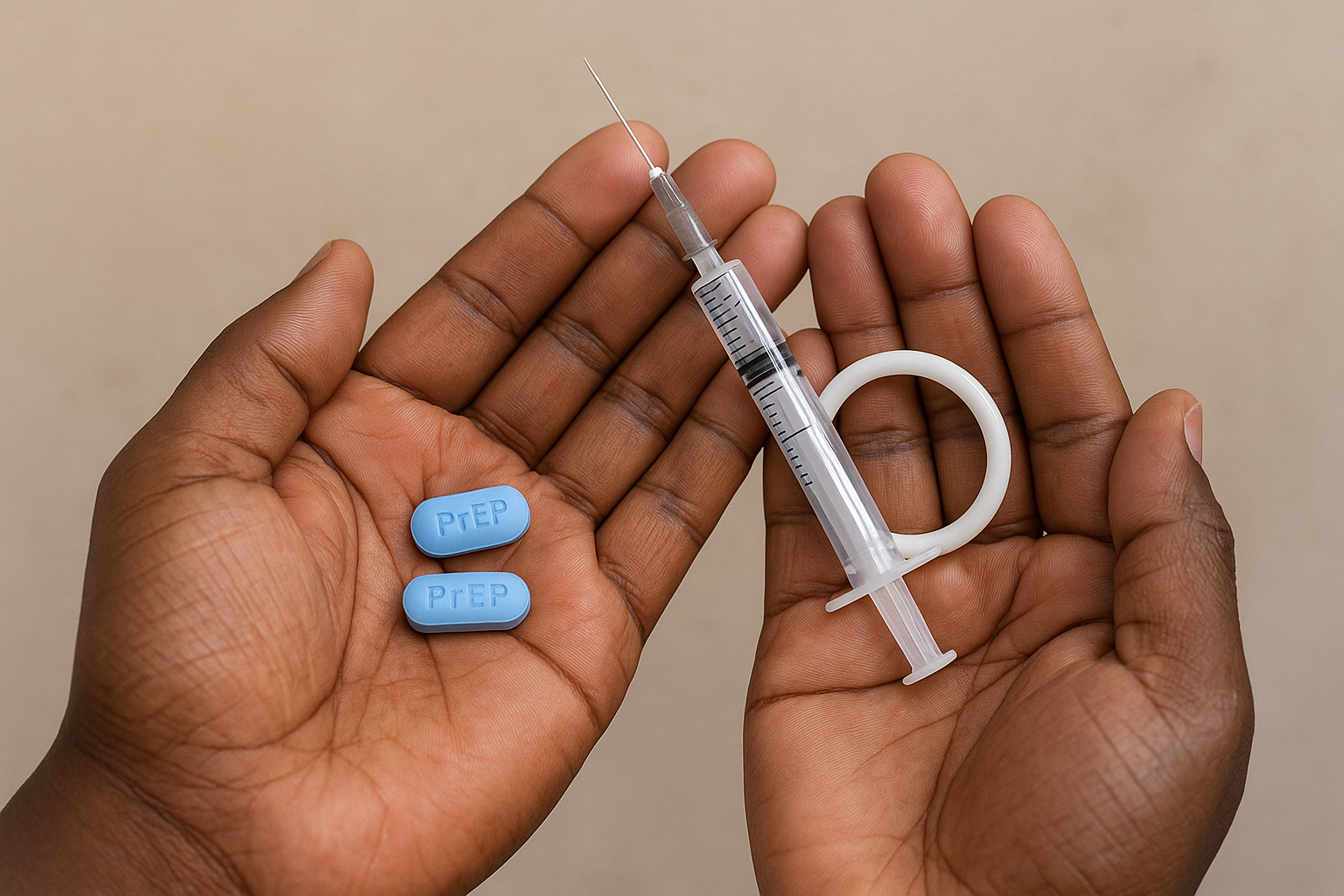
These services included the distribution of condoms, lubricant gel, HIV testing, antiretroviral treatment, and Pre-Exposure Prophylaxis (PrEP).
Community dialogues brought together sex workers, healthcare providers, law enforcement, and government institutions to address violence, rights violations, and barriers to care.
While health facilities continue to provide treatment, the weakening of community support systems has created significant service gaps.
“Health units continue to provide basic services for sex workers living with HIV, including antiretroviral treatment. However, monitoring of support groups for people with HIV has weakened due to a reduction in field staff, who previously supported the ongoing operation of PLHIV groups and served as a link between the community and health unit,” Mahumane says.
Mozambique has made important gains in treatment coverage. According to the CDC, 1,989,030 people were receiving ART in 2023. Viral load suppression among people enrolled in PEPFAR-supported treatment programmes reached 95% in 2024. However, the most significant impact of funding interruptions has been observed in prevention and outreach services.
“Since the funding interruption, there has been a reduction in field staff, resulting in insufficient personnel to provide outreach services, prevention messaging, and supplies in key locations, as well as to monitor cases of violence,” she explains.
These changes have made several essential services more difficult to access. “The services that have become difficult to access are those related to the follow-up of violence cases, the provision of prevention supplies, and the provision of PrEP.”
Despite these challenges, sex workers have demonstrated remarkable resilience.
“I have noticed positive changes, such as the strengthening of groups. They have become more united, more empathetic, and more welcoming,” Mahumane notes.
In the absence of formal support, communities have supported each other accompanying survivors of violence to police stations and health facilities, sharing information, and ensuring that no one faces violence alone.
Regarding HIV prevention, several options are available, including male and female condoms and oral PrEP. However, access to newer prevention technologies remains limited.
“The options that are easily accessible include male and female condoms and oral PrEP. Those that are not easy to obtain, as they are still in the pilot phase, include injectable PrEP.”
For Mahumane, real choice means having access to prevention methods that fit the realities of sex workers’ lives. However, many prevention options remain unavailable.
“It is frustrating to need a prevention method and not have it available. It feels as though providers are choosing methods for us. I would have liked to try vaginal PrEP, but it is not yet available in Mozambique.”
Her appeal to policymakers is urgent and unequivocal. “The primary need is the legalisation of sex work. We require specific legislation governing sex work that includes sanctions for those who violate our rights.” She also advocates for expanded prevention options.
“Introducing and making long-term prevention methods available to all is essential. This approach ensures inclusivity and can lead to greater adherence among beneficiaries.”
As Mozambique continues its HIV response, Mahumane’s message is clear: Sex workers must have the right, the resources, and the autonomy to choose how they protect their health. Without such a choice, HIV prevention efforts remain incomplete.